In digital dentistry, one of the most expensive and disruptive problems is the remake. A restoration remake affects every part of the workflow: it wastes lab resources, consumes clinician chairside time, delays treatment plans, and frustrates patients. Even high-performing dental labs struggle with remakes because the underlying causes are complex — incomplete data, unclear margins, inaccurate shade photos, last-minute changes, communication delays, or lack of structured workflows.
Digital Case Coordination is the modern answer to this challenge. Instead of treating each case as an isolated transaction, Digital Case Coordination turns dental workflows into a closed-loop ecosystem where data clarity, communication structure, and proactive verification significantly reduce errors before they occur. At VCAD Dental Outsourcing Lab, Digital Case Coordination is not a single role — it is a coordinated network of automation, human oversight, communication systems, and data-driven feedback cycles that together minimize remake rates and improve clinical outcomes.
This article analyzes how VCAD’s Digital Case Coordination system works and why it is central to delivering predictable, low-remake digital dentistry for global partners.
Most remake problems are predictable — and preventable. The key is understanding where errors originate before blaming design or manufacturing.
Missing interproximal surfaces, distorted occlusion, or unclear margins lead to design inaccuracies that cannot be corrected later.
Instructions like “slightly adjust contact” or “more translucency” look simple but result in misinterpretation, especially across time zones.
Improper lighting, absence of calibration cards, or incorrect shade photography cause color mismatches that require remaking the entire restoration.
Two clinicians may want different contact tightness or morphology styles — but without detailed preference profiles, labs rely on assumption.
If a lab waits hours or days for clarification, production timelines exceed tolerance, and rushed cases carry higher error risks.
Using the wrong material for thin margins, underprepared surfaces, or high occlusal load situations often leads to fractures or poor esthetics.
When these problems stack together, remakes become inevitable.
Digital Case Coordination solves this by creating a layer of structured control between clinician and lab.
Digital Case Coordination at VCAD is built around the principle that precision begins with information, not manufacturing. Instead of relying solely on technicians, VCAD assigns each clinic a dedicated Case Coordinator trained in:
The coordinator becomes the “single brain” that oversees all case movement, ensuring no detail falls through the cracks.
But VCAD takes this further: Case Coordinators work inside a digital ecosystem supported by AI, automation, and structured protocols.
Together, they create a coordination system that is:
• fast
• consistent
• transparent
• measured
• predictive
This transforms remake reduction from hope into a repeatable system.
Below is how VCAD’s system works step-by-step, ensuring problems are caught early rather than after production.
The moment a clinician uploads a case, VCAD’s system runs automated checks:
Errors are flagged instantly, and the coordinator reviews them manually for context.
Human context is essential. The coordinator verifies:
If any information is missing, the coordinator requests clarification immediately — often before the clinician has even left the room.
VCAD stores preference profiles for each clinician:
These preferences are automatically loaded into the CAD design so technicians don’t rely on memory or guesswork.
During design, the coordinator stays connected with both the technician and clinician. This eliminates the classic “silent gap” where assumptions lead to errors.
Before milling, the coordinator verifies:
This prevents heavy grinding or non-seating restorations.
After milling and finishing, high-resolution QC images are uploaded into the case record. The coordinator ensures everything matches the prescription before packing.
This multi-layer coordination makes errors extremely unlikely.
While humans excel at understanding nuance, AI excels at detecting patterns and highlighting risks. VCAD merges both.
AI flags:
• thin margins
• over-tapered preps
• occlusal collisions
• missing scan segments
• shade inconsistencies
Humans interpret clinical intent and decide whether revision is needed.
VCAD’s models analyze thousands of past cases and predict remake risks based on:
• tooth type
• prep geometry
• material
• clinician patterns
• shade complexity
High-risk cases receive priority review.
The system gradually understands each clinician’s preferences better than they remember them themselves — producing consistent results across years.
Digital Case Coordination is not a static workflow; it is an intelligent feedback system.
VCAD’s approach reduces remakes by attacking the problem at every stage.
Most remakes occur because errors slip through early stages. By applying strict intake and pre-design validation, VCAD removes the root cause.
Instead of vague instructions, all communication is structured:
• annotated 3D viewers
• standardized shade forms
• digital Rx templates
• visual feedback loops
Technicians no longer create designs based on assumption. Everything follows documented preferences.
When the crown fits with minimal adjustment, both clinicians and patients are happy.
Every remake case is analyzed and added into the VCAD intelligence system, preventing the same errors in future cases.
This is why VCAD maintains one of the lowest remake rates among global outsourcing labs.
Remake reduction is not the result of luck, talent, or better milling machines — it is the outcome of coordinated systems that protect information accuracy from the moment a case enters the workflow. VCAD’s Digital Case Coordination combines automation, human expertise, data intelligence, and structured communication to eliminate errors before they reach production. For clinicians, this means restorations that seat easily, esthetics that match predictably, and treatment schedules that stay on track. For DSOs and multi-location clinics, it means consistency across branches and a dramatically reduced operational burden. For patients, it means confidence — the restoration they receive is the restoration intended. With Digital Case Coordination, VCAD transforms precision into a guaranteed outcome rather than a hopeful expectation.
Digital Case Coordination is the modern answer to this challenge. Instead of treating each case as an isolated transaction, Digital Case Coordination turns dental workflows into a closed-loop ecosystem where data clarity, communication structure, and proactive verification significantly reduce errors before they occur. At VCAD Dental Outsourcing Lab, Digital Case Coordination is not a single role — it is a coordinated network of automation, human oversight, communication systems, and data-driven feedback cycles that together minimize remake rates and improve clinical outcomes.
This article analyzes how VCAD’s Digital Case Coordination system works and why it is central to delivering predictable, low-remake digital dentistry for global partners.
1. Why Remakes Happen — Understanding the Root Causes
Most remake problems are predictable — and preventable. The key is understanding where errors originate before blaming design or manufacturing.
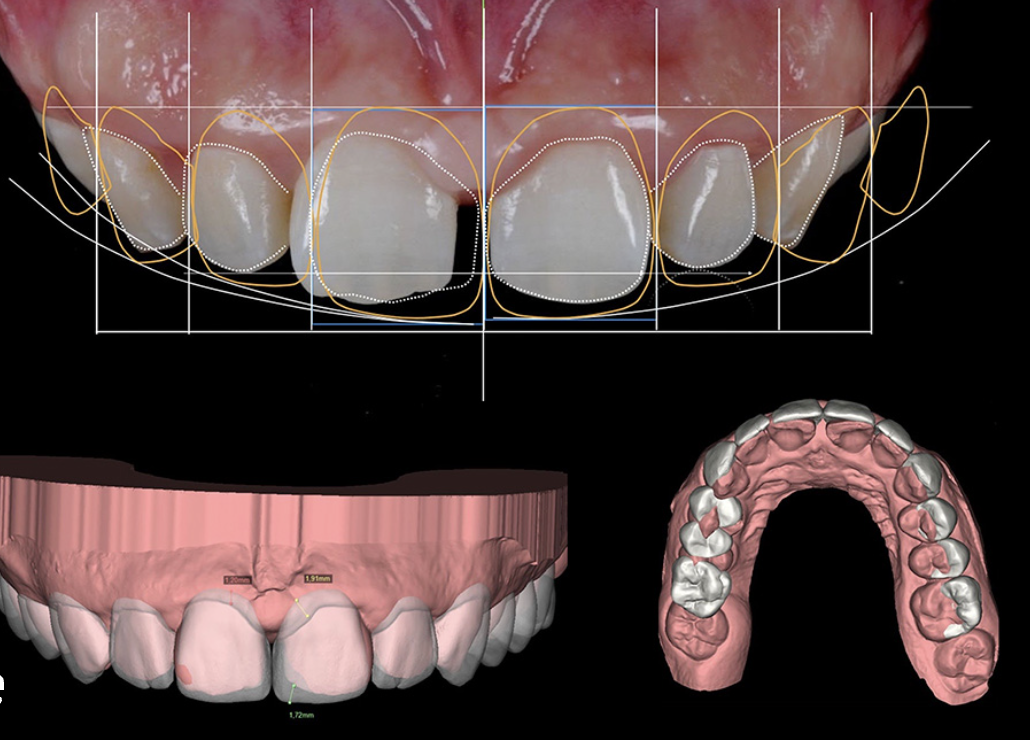
1.1. Incomplete or distorted scan data
Missing interproximal surfaces, distorted occlusion, or unclear margins lead to design inaccuracies that cannot be corrected later.
1.2. Ambiguous clinical instructions
Instructions like “slightly adjust contact” or “more translucency” look simple but result in misinterpretation, especially across time zones.
1.3. Shade inconsistencies
Improper lighting, absence of calibration cards, or incorrect shade photography cause color mismatches that require remaking the entire restoration.
1.4. Clinician preference variations
Two clinicians may want different contact tightness or morphology styles — but without detailed preference profiles, labs rely on assumption.
1.5. Communication delays
If a lab waits hours or days for clarification, production timelines exceed tolerance, and rushed cases carry higher error risks.
1.6. Material selection conflicts
Using the wrong material for thin margins, underprepared surfaces, or high occlusal load situations often leads to fractures or poor esthetics.
When these problems stack together, remakes become inevitable.
Digital Case Coordination solves this by creating a layer of structured control between clinician and lab.
2. What Digital Case Coordination Actually Means
Digital Case Coordination at VCAD is built around the principle that precision begins with information, not manufacturing. Instead of relying solely on technicians, VCAD assigns each clinic a dedicated Case Coordinator trained in:
- clinical terminology
• CAD/CAM workflows
• occlusal logic
• material selection
• communication strategy
• cross-department scheduling
The coordinator becomes the “single brain” that oversees all case movement, ensuring no detail falls through the cracks.
But VCAD takes this further: Case Coordinators work inside a digital ecosystem supported by AI, automation, and structured protocols.
Together, they create a coordination system that is:
• fast
• consistent
• transparent
• measured
• predictive
This transforms remake reduction from hope into a repeatable system.
3. The VCAD Digital Case Coordination Workflow
Below is how VCAD’s system works step-by-step, ensuring problems are caught early rather than after production.
3.1. Automated Data Verification (Intake Level)
The moment a clinician uploads a case, VCAD’s system runs automated checks:
- margin detectability
• occlusion alignment
• bite integrity
• scan completeness
• file corruption
• prep reduction analysis
• material compatibility
Errors are flagged instantly, and the coordinator reviews them manually for context.
3.2. Coordinator-Level Clinical Review
Human context is essential. The coordinator verifies:
- prep design vs chosen material
• shade consistency across images
• restorative category accuracy
• special instructions alignment
• patient esthetic expectations
If any information is missing, the coordinator requests clarification immediately — often before the clinician has even left the room.
3.3. Preference Matching
VCAD stores preference profiles for each clinician:
- contact tightness
• occlusal scheme
• morphology style
• emergence profile
• translucency and incisal halo effects
These preferences are automatically loaded into the CAD design so technicians don’t rely on memory or guesswork.
3.4. Live Communication Loop
During design, the coordinator stays connected with both the technician and clinician. This eliminates the classic “silent gap” where assumptions lead to errors.
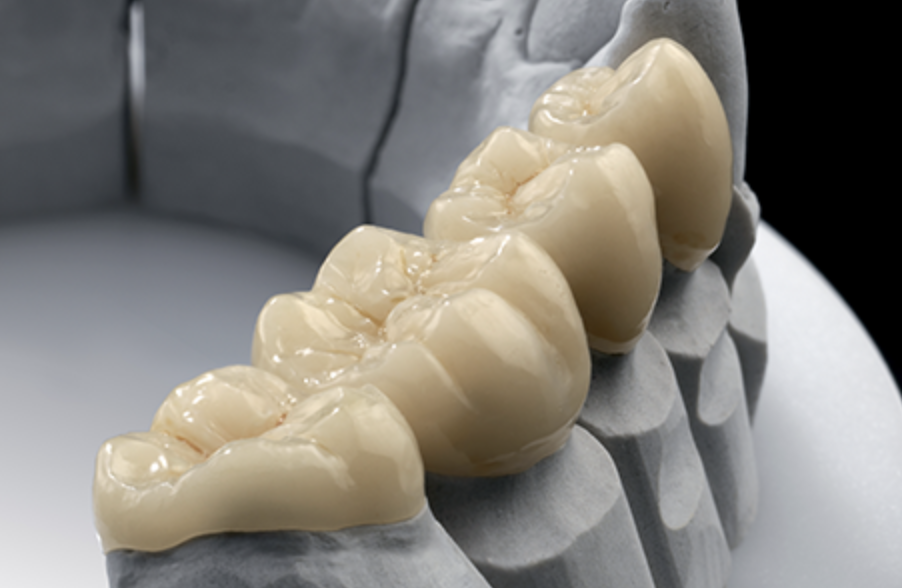
3.5. Pre-QC Structural Review
Before milling, the coordinator verifies:
- crown thickness
• connector design
• occlusal contacts under dynamic motion
• esthetic parameters
• scanned arch alignment
This prevents heavy grinding or non-seating restorations.
3.6. Post-QC Photographic Validation
After milling and finishing, high-resolution QC images are uploaded into the case record. The coordinator ensures everything matches the prescription before packing.
This multi-layer coordination makes errors extremely unlikely.
4. AI + Human Coordination: A Hybrid Model That Works
While humans excel at understanding nuance, AI excels at detecting patterns and highlighting risks. VCAD merges both.
4.1. AI Flags, Humans Interpret
AI flags:
• thin margins
• over-tapered preps
• occlusal collisions
• missing scan segments
• shade inconsistencies
Humans interpret clinical intent and decide whether revision is needed.
4.2. AI Predicts Remake Probability
VCAD’s models analyze thousands of past cases and predict remake risks based on:
• tooth type
• prep geometry
• material
• clinician patterns
• shade complexity
High-risk cases receive priority review.
4.3. AI Learns Clinician Patterns Over Time
The system gradually understands each clinician’s preferences better than they remember them themselves — producing consistent results across years.
Digital Case Coordination is not a static workflow; it is an intelligent feedback system.
5. How Digital Case Coordination Reduces Remake Rates
VCAD’s approach reduces remakes by attacking the problem at every stage.
5.1. Problems are prevented, not corrected
Most remakes occur because errors slip through early stages. By applying strict intake and pre-design validation, VCAD removes the root cause.
5.2. Communication becomes precise
Instead of vague instructions, all communication is structured:
• annotated 3D viewers
• standardized shade forms
• digital Rx templates
• visual feedback loops
5.3. Clinician expectations are stored and respected
Technicians no longer create designs based on assumption. Everything follows documented preferences.
5.4. Reduced chairside adjustment = reduced remake requests
When the crown fits with minimal adjustment, both clinicians and patients are happy.
5.5. Data-driven improvement
Every remake case is analyzed and added into the VCAD intelligence system, preventing the same errors in future cases.
This is why VCAD maintains one of the lowest remake rates among global outsourcing labs.
Remake reduction is not the result of luck, talent, or better milling machines — it is the outcome of coordinated systems that protect information accuracy from the moment a case enters the workflow. VCAD’s Digital Case Coordination combines automation, human expertise, data intelligence, and structured communication to eliminate errors before they reach production. For clinicians, this means restorations that seat easily, esthetics that match predictably, and treatment schedules that stay on track. For DSOs and multi-location clinics, it means consistency across branches and a dramatically reduced operational burden. For patients, it means confidence — the restoration they receive is the restoration intended. With Digital Case Coordination, VCAD transforms precision into a guaranteed outcome rather than a hopeful expectation.